PTSD vs Acute Stress Disorder: When to Test
January 26, 2026 | By Henry Davis
Feeling overwhelmed after a traumatic event? It's a natural human response, but it can be confusing and distressing when those feelings linger. You might be wondering, is what I'm feeling a temporary stress reaction, or could it be something more persistent? Many people who experience trauma find it difficult to tell if their symptoms will fade or if they signal a more serious condition.
Figuring out whether you're experiencing Acute Stress Disorder or PTSD can help you identify the right path forward for your healing journey. This knowledge helps you recognize when your symptoms need attention and when it might be time to seek a professional screening. This article will explain the timeline differences, symptom variations, and when you should consider taking a confidential PTSD screening test. Knowing what you are facing is the first step toward getting the right support.

Understanding PTSD and Acute Stress Disorder
To make sense of your experiences, it’s helpful to understand the clinical definitions of both Acute Stress Disorder and PTSD. They share many symptoms, but the key difference lies in how long those symptoms last. This distinction is vital for determining the right path forward.
Defining Acute Stress Disorder: Symptoms and Timeline
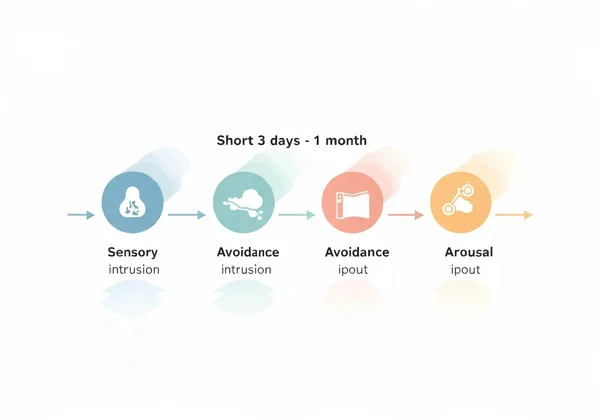
Acute Stress Disorder (ASD) is a mental health condition that can occur in the immediate aftermath of a traumatic event. The American Psychiatric Association's DSM-5 defines it as a set of symptoms that appear within three days to one month following the trauma. Think of it as the mind and body's intense, initial reaction to an overwhelming experience.
Common symptoms of ASD fall into several categories:
- Intrusion: Unwanted, upsetting memories, flashbacks, or nightmares about the event.
- Negative Mood: A persistent inability to experience positive emotions like happiness or love.
- Dissociation: Feeling detached from yourself, your thoughts, or your surroundings, as if you're in a daze. You might also have trouble remembering parts of the traumatic event.
- Avoidance: Actively avoiding distressing memories, thoughts, feelings, or external reminders (people, places, conversations) related to the trauma.
- Arousal: Difficulty sleeping, being easily startled, feeling constantly on edge, or having angry outbursts.
For many, ASD symptoms naturally decrease and resolve within a month. Early support during this phase can be highly beneficial.
PTSD Diagnosis Criteria: From One Month Onward
PTSD is diagnosed when trauma-related stress symptoms persist for more than one month after the event. Often, PTSD develops when Acute Stress Disorder doesn't resolve on its own. These symptoms may appear directly after the trauma or even months or years later.
According to the DSM-5, a PTSD diagnosis requires symptoms from four specific clusters:
- Intrusion: Similar to ASD, this includes recurrent distressing memories, dreams, or flashbacks.
- Avoidance: Persistent effort to avoid internal memories or external reminders of the trauma.
- Negative Alterations in Cognition and Mood: This is a broader category that includes memory problems, negative beliefs about oneself or the world, persistent fear or anger, and feeling detached from others.
- Arousal and Reactivity: This includes irritable behavior, reckless actions, hypervigilance (being overly alert for danger), an exaggerated startle response, and trouble concentrating or sleeping.
If your symptoms last longer than a month and are causing significant distress, a PTSD self test can provide valuable initial insights.
Key Differences Between PTSD and Acute Stress Disorder
While the symptoms can feel very similar, the clinical distinction between ASD and PTSD is important. Understanding these differences can help you frame your experience and know when to seek further evaluation. The two main factors that set them apart are the timeline and the overall impact on your daily life.
Timeline Distinctions: The One-Month Marker
The most clear-cut difference between ASD and PTSD is time. ASD is a short-term condition, with symptoms lasting from three days to one month after a traumatic event. In contrast, PTSD is a long-term condition, diagnosed only when symptoms persist for longer than one month.
This one-month marker is clinically significant. Many people experience trauma symptoms immediately after an event, but their minds and bodies naturally begin to heal. The symptoms may lessen and disappear without turning into PTSD. However, if the symptoms don't improve or even worsen after a month, it suggests the stress response has become chronic and may have evolved into PTSD. For example, someone who experiences flashbacks and anxiety for two weeks after a car accident may have ASD. If those same symptoms are still present and disruptive two months later, a professional would then consider a PTSD diagnosis.
Symptom Severity and Functional Impact
While both conditions are distressing, PTSD is often associated with a more significant and lasting impact on a person's ability to function. The symptoms of ASD, while severe, are often viewed within the context of an immediate crisis response.
PTSD's chronic symptoms can significantly impact major areas of life. For example, persistent avoidance and emotional numbness may strain relationships with family and friends. Meanwhile, hypervigilance and concentration problems can make it difficult to maintain employment or succeed in school. Over time, these functional impairments can become more pronounced than they might be during the initial one-month ASD period. It's crucial to take any thoughts of self-harm or severe dissociation seriously, as these can be present in both conditions and require immediate professional help.
When to Take a PTSD Screening Test
Knowing the difference between ASD and PTSD is helpful, but how do you know when it’s time to take the next step? A screening test is a tool designed to help you organize your symptoms and understand if they align with the criteria for PTSD. It’s a private, confidential way to get clarity.
Signs That Your Stress Response May Be Becoming Chronic
If you are past the one-month mark and your symptoms aren't getting better, it’s a strong indicator that you should look closer at your experience. Ask yourself these questions:
- Are my symptoms staying the same or getting worse over time?
- Am I avoiding more places, people, or activities than I was a few weeks ago?
- Do I feel just as jumpy, on edge, or irritable as I did right after the event?
- Is it becoming harder to connect with loved ones or feel positive emotions?
- Are my sleep, work, or relationships suffering because of how I feel?
If you answered "yes" to one or more of these, your stress response may be becoming chronic. Recognizing this is not a sign of weakness; it's a sign of self-awareness. It's an opportunity to take proactive steps toward healing, and a confidential assessment is an excellent place to start.

Taking the Next Step: What to Expect from PTSD Screening
A PTSD screening test, like the PCL-5 (PTSD Checklist for DSM-5) that our tool is based on, is a questionnaire that measures the symptoms you've experienced over the past month. It asks you to rate how much you have been bothered by specific issues, such as unwanted memories, avoidance behaviors, and feelings of alertness.
It's important to note that an online screening test isn't a formal diagnosis. Only qualified healthcare professionals like psychiatrists, psychologists, or therapists can provide an official diagnosis. However, screening tools are valuable first steps. They offer a structured way to review your symptoms and provide results that help determine your next steps. You can take your results to a doctor or therapist to start a conversation, giving them a clear picture of what you've been going through.
Understanding Your Experience After Trauma
Telling the difference between ASD and PTSD matters not just clinically, but personally—it's about making sense of your own experience after trauma. ASD is an immediate, intense reaction that often subsides within a month. PTSD is diagnosed when those symptoms persist, becoming a chronic condition that affects your daily life.
Remember, understanding your condition is the first, most powerful step you can take toward healing. Both ASD and PTSD are treatable, and you do not have to navigate this path alone. By seeking clarity, you open the door to effective support and strategies that can help you reclaim your sense of safety and well-being.
Are you ready to gain a clearer picture of your symptoms? Take our free, confidential PTSD test today to better understand your trauma response and explore your next steps toward recovery.
Frequently Asked Questions About PTSD and Acute Stress Disorder
Can I develop PTSD without first having Acute Stress Disorder?
Yes, it is possible. While many people with PTSD initially meet the criteria for ASD, some may not. PTSD symptoms can sometimes have a delayed onset, appearing more than six months after the traumatic event. Certain risk factors, like the severity of the trauma, lack of social support, or a history of previous trauma, can increase the likelihood of developing PTSD directly.
How accurate are online PTSD screening tests?
High-quality online screening tests, especially those based on clinically recognized tools like the PCL-5, can be very accurate for screening purposes. They are designed to identify whether your symptoms are consistent with the criteria for PTSD. However, they are not a substitute for a professional diagnosis. If your results from an online PTSD test indicate a potential issue, it is a strong signal that you should speak with a healthcare provider for a full evaluation.
What treatments are available for ASD and PTSD?
Both conditions are treatable with evidence-based therapies. For ASD, early intervention with trauma-focused cognitive-behavioral therapy (CBT) can be effective and may even prevent the progression to PTSD. For PTSD, leading treatments include therapies like CBT, Eye Movement Desensitization and Reprocessing (EMDR), and Prolonged Exposure (PE) therapy. Medication may also be recommended by a psychiatrist to help manage specific symptoms.
Is it normal to feel worse after learning about these conditions?
Yes, it can be. Learning about trauma-related conditions can sometimes bring up difficult feelings or make you more aware of your own symptoms, which can feel unsettling. This is a common and normal reaction. It shows you are confronting your experience, which is a courageous step. However, if this worry becomes overwhelming, it's another important sign that reaching out to a mental health professional for support is a good idea.